Geography
| Task | Location |
|---|---|
| Home ward | 1 West – Orthopaedic surgery ward – the bulk of your orthopaedic surgery patients 3 B – OrthoGeris ward – the bulk of postop neck of femur fracture patients |
| Morning meeting point | 0700 in the Ortho Registrar offices Level 1 (door code is on door frame) —Except Friday handover is at 0630 (because Unit Radiology Meeting in Mitchell Mavis Room or Auditorium is at 0700) —Sometimes Friday handover is at 0700 due to the radiology meeting being later |
| Your pager | Each HMO/Intern receives their own pager which you have for the entirety of the rotation; you should hypothetically only get paged when you’re on the ward (on ward week) — Please check with Switch before commencing your rotation — You should always write your pager number on the 1 West whiteboard |
| Patient list | ~10-40 patients (patients under Ortho and OrthoGeris bedcards) |
| Handover | 0700 in the Ortho Registrar offices Level 1 –except Friday’s handover is at 0630, because Unit Meeting in Mitchell Mavis Room is at 0700 |
| Outpatient Clinic | Tuesday – AM Wound Clinic (HMO/intern) – PM Fracture Clinic (HMO) Friday – AM Consultant Clinic (HMO/intern) – AM Registrar Clinic (HMO/intern) runs concurrently with consultant clinic |
| RMO Quarters | Footscray – Level 3, enter via lifts in front of ED (swipe card needed) Sunshine – Level 1, opposite birth suite, corridor between ICU and theatre (code written on door) Williamstown – Level 1, corridor leading away from upper GEM |
About the Role
- The FH orthopaedic team primarily takes care of adult and geriatric ortho patients (a significant inpatient and outpatient caseload)
- These mostly consist of trauma cases, but sometimes will also consist of elective cases
- The rotation is a mix of inpatient and outpatient duties and is conveniently divided into the “ward week” and “clinic and PAC follow up week”
- Make sure the Footscray trauma excel sheet (front sheet) is printed once it has been updated (by the morning reg) and stapled to the audit sheet (which should have a list of current inpatients).
- Please familiarise yourself with adding patients to the audit
- Ward round notes are taken on paper (we traditionally do not take a WOW on the round), and then transcribe notes onto EMR later
- When seeing a new patient, bring a consent form and a marking pen and an ARP form (for adult patients) – super handy!
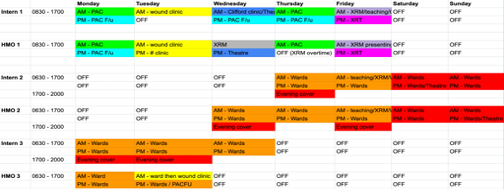
- There is a 3 weeks rotating roster:
- Ward Week – 7 days Wednesday -Tuesday (for HMOs) and Thursday – Wednesday (for interns) on the wards
- Clinic Week – 5 days (Mon-Friday)
- The default fall back on any given day if you are not busy or finished doing your delegated jobs is to help out the ward person. They always have stuff to do.
- Days off (9 days out of every 21 days)
Attendance in the Operating Theatre
- This is encouraged by all the consultants, and everyone is welcome to attend
- However, ward duties must be performed first in a timely manner and someone (intern/HMO) should be on the wards to cover for UCRs/MET calls and be present for timely reviews if there are nursing concerns
Responsibilities
- The responsibilities can be broken down into ward week and clinic week
Ward Week
0630 – Pre-Round Preparation (Orthopaedics Registrar Office – Level 1)
- Take handover from the night HMO (in person or via the “I’m Special” Whatsapp group
- Interns/HMOs update the audit (which is our unit-specific handover sheet, please read the HMO page to see how to do this). This includes:
- Adding in updates regarding patient status (i.e. UCR/MET calls, significant events overnight, etc.)
- Updated bloods
- Operation details and postop orders (and adjusting the consultant name to the appropriate consultant)
- Patient comorbidities
- Staple the Google Drive front sheet to the printed audit ward list
0700 – Handover (Orthopaedics Registrar Office – Level 1)
- Take notes of the plans for outpatients on the front sheet as well as inpatients on the audit sheet as the ward round usually goes by relatively fast and plans don’t tend to change significantly after handover
- Be especially cautious regarding Operating Theatre lists and fasting times and document accordingly on ward round note
- HMO should handover any updates for the inpatients, including major events overnight, opinions of consulting teams and especially D/C planning (destination, timing, barriers)
0730 – Ward Round (1 West and non 1 West (typically 3B))
- Split into 2 teams (1 West and non 1 West)
- NIC + Allied Health on 1 West need to be notified when you start the ward round + NIC on 3B (orthogeris ward)
- Can be quite fast – some HMOs consider having a laptop on wheels to be useful, others like writing notes down on paper
- Documentation: ensure you document using EMR using proforma (ask current resident how to add autotext to your EMR profile)
- Important checklist items to include in your documentation are:
- Anticoagulation status/DVT prophylaxis
- Antibiotics
- Aperients
- Fasting status
- Weight bearing status
- Neurovascular status (please check with registrars or consult an anatomy textbook to ensure accurate documentation)
- Upper limb: axillary, musculocutaneous, median, ulnar, radial nerves sensation and motor function
- Lower limb: femoral, superficial peroneal, deep peroneal, tibial nerve sensation and motor function, lateral femoral cutaneous, sural, saphenous sensation
- Important checklist items to include in your documentation are:
- 3B team attends OGS meeting on 3B (around 0830)
- Everyone then attends Coffee Round – the most senior person will buy everyone coffee, held in Greenbag
0800 onwards – Ward Duties
Priorities (see below for elaboration)
- Pre op patients for current day
- Discharges and transfers (scripts are priority, summaries and clinic bookings can be performed later
- Submit accurate documentation of ward round notes (see above)
- Chasing and posting postop scans in team chat (Whatsapp)
- Referrals and scans
- 1200 Allied Health meeting – 1 West at the end of the corridor
- Remainder of jobs
Pre-op Patients
Checklist
- Valid consent (HMO/Registrar responsibility)
- Side/site is marked
- Booking (EMR order for “request for emergency surgery” and discussion with OT NIC x56168 regarding which theatre list they will be on)
- Up to date imaging: Xrays and advance imaging if required
- Anaesthetics discussion – all pre-op patients should be discussed with anaesthetics in charge x56540
- If they advise a formal review then page the APMS registrar and submit an EMR referral for “consult to medical specialty” with “anaesthetics and periop medicine” as the consulting team for a formal, in-person preoperative review.
- Valid Group and Hold (G&H) if required – For all major surgeries (check with HMO/Registrar if unsure, follows PAC guidelines)
- Pre-op bloods
- Hb: general rule is >100 for all major surgeries but check with reg if <100
- Fasting Status
- Ensure the patient is appropriately fasted and the bedside nurse and the NIC are aware of fasting status
- Ensure it is documented correctly and the ward has been appropriately updated (simply documenting is NOT sufficient)
Pre-op Orthogeriatric Neck of Femur Fracture (NOFF) Patients
- In addition to the above, NOF patients need a few additional considerations given they are a higher risk cohort and more frail population
- EMR Booking needs to be done AS SOON AS they are seen (evening/night HMO can do this)
- ARP form or resuscitation status must be done on admission (intern should pass this on to the night cover if admitting)
- Informed Consent may need to be done via the next of kin or a medical treatment decision maker if the patient lacks capacity
- Next of kin should be updated on admission
- ALL patients need to be discussed with the anaesthetist in charge as soon as practical
- ALL patients need to be reviewed by the orthogeriatrics team for medical optimisation preop or discussed/reviewed by the senior gen med registrar (clinical lead) after hours
- A full set of geriatric bloods should be done on admission (including coagulation studies and a group and hold)
- These patients are admitted under the Orthogeriatrics/Acute Aged Care team during normal hours and after hours, the Orthopaedic surgery team looks after them
- Also please ensure that you are in the OGS Slack communications chat as that is where you will directly communicate with the OGS teams about pre and postop NOFF patients
- Download the Slack app through the WH Apps site on the intranet and ensure that you download the Slack-WH clinicians app, then request an admin (someone from either team) to add you to the OGS chat
Discharges
- Discharge scripts and medication reconciliations are most important thing to complete in the morning, summaries and clinic bookings can be done later in the day
- If patients are being transferred to a different hospital, ensure that the transfer summary is also completed promptly
- On weekdays you only need to do discharges for Orthopaedic surgery patients not Orthogeris patients (on weekends you cover orthogeris as well so may have to discharge them)
- Patients who are non-weight bearing in their lower limbs must go home on DVT prophylaxis for the duration of their NWB period (could be aspirin or enoxaparin and occasionally a NOAC)
- Most ortho patients get a wound review 2/52 post op and fracture or consultant clinic 6/52 post op – HOWEVER confirm with instructions on the op note as it is sometimes different)
- To refer on EMR, place the following order:
- OP Orthopaedic wound referral
- It is important to mark the referral as URGENT otherwise the admin staff will not pass this on in time to the clinics bookings nurses
- OP Orthopaedic fracture referral
- OP Orthopaedic consultant referral
- Exception: most NOFs have no ortho follow-up they just get a wound review in 2/52 post op with LMO
- OP Orthopaedic wound referral
- ERAS patients (NEW)
- See ERAS page for protocol and booking followup
- In summary, for patients who are in catchment (excel list on ERAS page), they get booked on BossNet. For patients who are out of catchment, they get booked through an EMR referral as usual
Postop scans/bloods
- For patients that have a day 1 xray as part of their postop plan, ensure this has been ordered prior to the ward round starting (ideally ordered day of surgery for the next day)
- Chase the scan and post it in the team group chat (Whatsapp) and tag the registrars involved
- If postop bloods were ordered or requested, chase those and post that information alongside the scan
Referrals and scans
- It is important to send out pages early as it can take a while to get a call back – additionally, from an orthopaedic perspective patients are usually cleared for discharge pretty quickly and medical/AH issues are barriers to discharge (there will be a lot of pressure on you to get medical issues sorted to get patients to the next destination)
- You will be discussing with ID and gen med regularly
- For longer staying/complex Orthopaedic surgery patients, it is good practice to flag with SNAP early for discharge planning purposes (Nurse usually refer to SNAP so ask in the AH meeting if we can refer to SNAP)
- Note: the orthogeris team will manage the medical issues for pre/postop NOF patients on weekdays
Allied Health Meeting
- 1200 every weekday in room at the end of 1W
- Attendees include: JMOs on the orthopaedic unit, NUM, NIC, physiotherapists, occupational therapists, social workers, bed coordinators
- You will lead the discussion by letting everyone in the room know
- Who the patient is
- What their orthopaedic issue is (pre/postop)
- What their demographics are (from home, from nursing home, with supports)
- and then gather information regarding their discharge planning progress
- Discharge planning is most important information to take from this meeting > needs to be updated on the audit and handed over in the morning e.g. “aiming GEM” or “W/L for GEM” or “aiming home” etc.
- The equivalent meeting occurs at 0830 on 3B every weekday for all OGS patients
Other Ward Duties
- Postop Day 1 patients
- Ensure bloods and xray have been done and the registrars involved have been updated
- Ensure that appropriate antibiotics have been charted if required (commonly 2g cefazolin for 2 further doses 8 hrly postop or clindamycin 600mg if severe allergy)
- Check that the appropriate DVT prophylaxis has been charted
- Usually 40mg enoxaparin at 2000 every 24 hours, but dose adjust according to patient weight according to WH guidelines
- Check that TXA has been charted if on postop orders
- Ensure NOF patients have regular aperients charted and bowels open regularly
- 2x movicol BD, 2x docusate senna BD is recommended
- Ensure anaemia is addressed
- Identify the source of bleeding/reason for anaemia
- In general, aim Hb>80 if no history of IHD
- If history of IHD, we would usually aim Hb>100, but discuss this with the registrar/in consultation with the medical team if required
- This may mean the patient gets one or more blood transfusions
- Ordering bloods
- Rationalise ordering bloods! This is a common pitfall
- All postop patients should get an FBE and UEC on day 1, and potentially day 2 if required and no further unless they are deranged or something else needs to be monitored
- Patients with active infections (acute/chronic) should ideally get a 2nd daily CRP unless the registrar wants one sooner
- Patients on long term antibiotics which are metabolised through the hepatic portal venous system (e.g. fluclox) should get LFTs checked
- Hub and spoking imaging
- Chasing correspondence
- Chasing operation notes, implant details, nurse count sheets from other health networks
- If arthroplasty details are not easy to obtain, you can call and email the Australian Orthopaedic Association National Joint Replacement Registry (AOANJRR) with their template referral form to get details
- E: admin@aoanjrr.org.au
T: +61 8 8128 4280
Cover shifts
- On 2 days of the ward week you will be on cover, which means you will be covering all of orthopaedic surgery and the orthogeris patients from 1700-2030
- The OGS teams will communicate any handover to you via the “Slack chat”
- You will need to be added to it by finding Slack and registering on WH Apps (through the intranet)
- Hand over to night cover either in ressies or over the “I’m special” WhatsApp group
On the Weekend
- On weekends Ortho covers OGS patients as well. There is no OGS team on the weekend
- Friday night – get a handover from the OGS teams 4pm at AAC5 office on 3B. Make sure medically unstable patients are on the list for registrar review over the weekend.
- Ask the weekend Ortho reg what time they want to start rounds, its reg and theatre dependent; although it’s usually been same as during the week – 0700 handover.
Otherwise weekend works the same as a weekday
clinic week
- Clinic week consists of a few responsibilities which revolve around attending and preparing clinics, as well as following up on patients who are booked to surgery. These include:
- Pre-admission clinic (PAC) (Monday and Thursday)
- Wound clinic (Tuesday)
- Fracture clinic (Tuesday)
- Mr Clifford clinic (Wednesday)
- Consultant clinic (Friday)
- PAC followup (remainder of time)
- Fracture clinic preparation (remainder of time)
- Other particulars include:
- Half day for the intern on Tuesdays
- Half day for the HMO on Thursdays
- Rostered theatre time for the HMO on Wednesday afternoons
Pre-admission Clinic (PAC)
- See the HMO guidelines section on PAC for more information on how to “PAC” a patient
- There are also orthopaedic specific guidelines on what bloods/investigations to order within the drawers in the rooms
- Essentially the purpose of PAC is to identify any medical/anaesthetic issues which may preclude a patient from surgery and to optimise them
- If these issues are too significant or a patient needs more time before surgery can proceed, then the unit needs to be informed and a “not ready for care” (NRFC) form needs to be completed
- You will run through a general checklist of their health and check their bloods and imaging as well as document medication advice as per perioperative guidelines (which can be found on PROMPT)
- There is a minor PAC on Monday mornings and major PAC on Thursday mornings
- Monday morning minor PAC is for seeing patients who have been waitlisted for minor to intermediate surgeries and have been flagged by the PAC nurses as higher risk
- Some patients booked to this clinic are just for followup or file reviews of pending investigations
- Thursday morning major PAC is for seeing patients who have been waitlisted for major surgeries and mostly consists of joint arthroplasties or patients who are significantly comorbid and need an anaesthetics review
- There will always be an anaesthetist there who will guide you with respect to further correspondence/investigations required and whether a patient is suitable to proceed
- If a patient is NRFC, then the registrar should be informed and the NRFC form completed
Wound clinic
- Tuesday morning Level 1 outpatients
- Usually patients booked here are 2 weeks postop
- Key things to review and document include:
- Check the wound, ensure that it is healing well
- If any wound concerns such as dehiscence or infection, raise this with the registrar involved in the case
- They might need an adjusted dressing plan, removal of part or none of their sutures, a period of oral antibiotics, change to their weightbearing status etc
- If wound concerns, consider reviewing the patient again the following week
- Check neurovascular status
- Check ROM for post total knee replacement patients
- Check the wound, ensure that it is healing well
- Ensure the rest of their postop orders are adhered to
- Ensure that plaster technician referrals are in place if required (they can do plaster/brace/splint/Cam boot applications/modifications/removals)
- Ensure that physiotherapy appointments are in place
- Ensure that followup appointments (fracture clinic or consultant clinic) are booked
- Ensure that the DNAs are sorted (phoned and rebooked or cancelled) by the end of the clinic
- In general we attempt to rebook them in almost all circumstances unless the patient chooses not to followup with us
- These need the “no show” option clicked on Ambulatory Organiser
Fracture clinic
- Tuesday afternoon Level 1 outpatients after wound clinic
- You will assist the registrars in seeing fracture clinic patients in the afternoon (generally because it is very overbooked and busy)
- Run every patient by a registrar or the trauma fellow in clinic after collecting all the information and formulating a plan
- There will be new patients who have been referred in by the GP/other units as well as review patients
- This is a great source of learning!
Mr Clifford clinic
- Mr Clifford sometimes has a clinic Wednesday mornings. Check the dates with Ambulatory Organiser and with the clinics bookings nurses
- The intern is generally assigned to this clinic
- There will usually be a registrar also assigned to the clinic
- Your role will primarily be to aid in the accurate documentation of patient reviews after seeing them with Mr Clifford
Consultant clinic
- Friday morning level 1 outpatients
- One HMO will be allocated to go to Clinic D to complete campus suitability assessment for patients who are going on the waiting list for a joint replacement
- Your role is to assist wherever possible. This may include
- Assisting consultants with ordering investigations or other jobs
- Seeing patients on behalf of consultants and then discussing them with them
- Assisting nurses with concerns
- This is also a great opportunity to learn and get to know bosses
PAC Follow up
- This is a job that occurs throughout the week during your free hours
- You will need to locate the “ORTHOPAEDICS 2024” excel sheet excel sheet that the surgical liaison nurses Jessy and Aleks use to book patients for surgery with. This is inside the “UNIT BOOKINGS” folder inside the Shared drive” of any computer
- The patients are then transcribed over to the “PAC FOLLOW UP” Google sheet located in the Western Ortho Google drive
- All patients listed in black on the SLN sheet should be transcribed over, which can be up to a month in the future
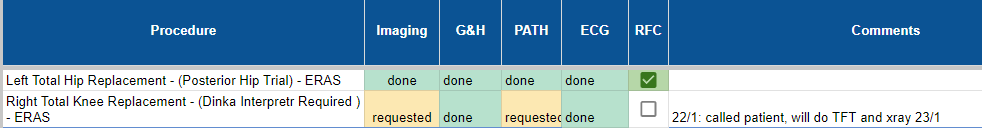
- You will then systematically go through their files and ensure that all their relevant investigations, including bloods, extended group and hold, xrays, ECGs are up to date
- It is very important that patients who require a group and hold get an EXTENDED GROUP AND HOLD so that their blood type is saved for 30 days rather than 72 hrs
- All diabetic patients should have a Hba1c <8.0%, and if not warrant a discussion with the registrar +/- endocrinology team or otherwise will be cancelled
- To determine what bloods and ECGs are required, use the “Guidelines for ordering basic pre-operative investigations” document located on PROMPT
- Some general pointers:
- Total joint arthroplasties require: ECGs, extended Group and Hold, recent (within 3 month) templated xrays and a full panel of bloods
- Arthroscopies (including arthroscopic ACL reconstructions) only require a recent xray (usually already have advance imaging like an MRI which needs to be hub and spoked) and no other bloods unless they are a comorbid patient
- Removal of metal procedures will require an xray and potentially a CT depending on the complexity of the procedure and basic bloods unless the patient has other comorbidities
- If there are concerns regarding their fitness for surgery (raised inflammatory markers on bloods, ECG abnormal), you should discuss this with the registrars and the anaesthetics in charge
- Do NOT order investigations for Mr Harris patients. He prefers to ensure they are ordered correctly himself.
Fracture clinic preparation (formerly known as XR triage)
This job entails ordering xrays, plaster technician referrals, chasing correspondence and hubbing and spoking relevant imaging for patients who will be seen in the Friday consultant clinics.
Key steps include:
- Generating the list of patients from “Ambulatory Organiser” on EMR
- On Monday, change the date to the upcoming Tuesday (next day)
- After Tuesday, change the date to the following Tuesday
- Ensure that “Ortho FH Fracture AM” and “Ortho FH Fracture PM” is ticked in the “Patients for: … ” text
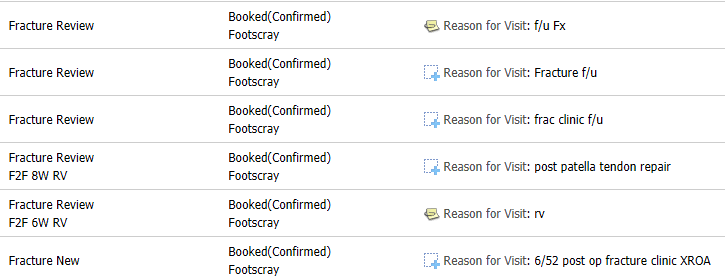
- Go through the list of new patients only (not reviews, as of Nov 2024, questions to reg Ben please) and check their Bossnet clinic notes/EMR notes/Bossnet GP referrals and ensure their imaging is up to date (pointers and protocols below)
- “Tick off” the new patients by writing a sticky note next to the patient in Ambulatory Organiser (this sticky note thing will hopefully be gone soon-ish, speak to reg Ben)
Acquiring imaging
– Generally the only imaging you can “order” for an upcoming patient will be xrays. This is because they can be done on the day of clinic
– Any advanced imaging such as ultrasound, CT, MRI, SPECT (bone scan), PET will usually be organised by the registrar or the referring GP/specialist and should be ordered/performed well in advance of the clinic
– Your job will be to acquire all the relevant imaging, either by ordering new xrays or chasing and collating all the other imaging (by hub-and-spoking them or calling and asking the patient to bring in CDs/reports of their imaging)
– The registrar triaging the patient will often have written what they would like done (can access on Bossnet)
Ordering X-rays and plaster tech referrals
These are some general guidelines for ordering xrays. Also it can be helpful to search the patient URN on Synapse to check if the previous clinician has already ordered an xray (to prevent duplication of orders)
For NEW patients (all REVIEW patients should have imaging and plaster tech orders from the registrar who saw the patient in clinic):
1. Order an xray if within 1-2 weeks of injury and first appointment in fracture clinic
2. Always order the joint xray for fractures/surgical fixations close to the joint (i.e. distal radius = wrist, proximal humerus = shoulder, tibial plateau = knee)
3. For distal radius fractures more than a few days old
– change from current slab to a moulded BEFG cast and xray in the new cast
4. For clavicle fractures, order an additional 15 deg cephalad view and consider xray of the contralateral side for comparison
5. For ankle fractures, get the patients out of plaster and get a weightbearing AP, mortise, lateral view and put them into a Cam boot
6. For foot fractures (i.e. simple metatarsal, phalangeal fractures), put them in a Cam boot and get xrays of the foot
7. For true scaphoid fractures, they will need immobilisation in a thumb spica cast and xray in the new cast with scaphoid views
8. For query fractures (including query scaphoid fractures), the patient should be taken out of plaster and xrays should be obtained as well as being clinically examined
Contributors and Authors
- Phong Tran 8/10/23
- Matthew Sun 24/01/24
- Ben McElwee Nov 2024
